Signs of osteoarthritis of the knee joint are often found in older people.Athletes and obese patients are also at risk.
Why does osteoarthritis of the knee joint occur?
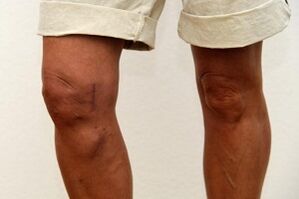
Osteoarthritis is a deformation of the articular cartilage.Cartilage acts as a shock absorber and facilitates the movements of the human body.When they are destroyed, mobility gradually decreases and any strain causes pain.Over time, the knee becomes completely immobile and the person may become disabled.
All cartilage thins and wears away with age, so the disease occurs in various stages in 70-85% of people over 60 years of age.These are primarily overweight women.Other common causes of osteoarthritis:
- Intensive sport and physical overload contribute to premature cartilage wear even at a young age.
- Injuries, fractures, dislocations.
- Genetic predisposition.
- Congenital disorders, lack of intra-articular fluid.
- A circulatory disorder in which the cartilage receives little oxygen and nutrients.
- Joint diseases that are accompanied by inflammation.
- Violation of hormone production and metabolism.
A form of osteoarthritis that affects the knee joint is called gonarthrosis, from the ancient Greek “goni” – knee.
Classification of arthrosis of the knee joint
There are 3 stages of this condition depending on the degree of osteoarthritis development.The earlier the disease is detected, the more successful and easier the treatment is.Characteristics of different stages of osteoarthritis:
- At this stage, the bone deformation is not yet pronounced.Abnormalities can be seen on x-rays, but few people pay attention to minor symptoms and go to the doctor.
- Changes and thickening of the bones can be seen with the naked eye on x-rays.The quality of life decreases due to constant complaints.
- The patient's movement is significantly restricted.Ligaments and cartilage are completely destroyed.
Many older people endure pain until the last moment and suffer from illnesses because they get used to age-related diseases and consider these symptoms normal.However, in the early stages you can cope with conservative methods; in the final stages, only surgery helps.
Main symptoms
The disease does not begin suddenly, but develops over several years.Mild pain in the knee is initially only felt under heavy strain, when going up and down stairs.If the osteoarthritis is not treated, the pain symptoms become permanent over time, the knee joint takes on an unnatural shape and contour and the leg can bend to the right or left.
At level 1
Long before serious osteoarthritis develops, you may experience mild knee discomfort after walking.Occasionally there is stiffness in movement and grinding.These symptoms should not be ignored, because with timely examination, treatment can be initiated and serious consequences can be prevented.
At level 2
At this stage, the patient feels almost constant pain.It is most pronounced in the morning, subsides after a short walk, but worsens in the evening.The patient's gait slows down, accompanied by a constant grinding sound.Redness and swelling of the skin often occur in the knee area, which indicates an inflammatory process.The x-ray shows clear changes.
diagnosis
An orthopedist examines and detects osteoarthritis of the knee joint.Diagnostics includes laboratory and instrumental research methods.This includes:
- Blood and urine tests.Show the level of hormones in the body and the presence of inflammation.
- Radiography.Helps assess joint type and determine disease stage.
- Magnetic resonance imaging.Shows the condition of soft tissues, meniscus and cartilage, which is not possible with x-ray.
- Ultrasound of joints.Like MRI, it shows the condition of the cartilage and surrounding tissue.This is a rather subjective method, the result depends on the qualifications of the specialist.An ultrasound examination should therefore be carried out in addition to magnetic resonance imaging.
- Personal inspection.Sometimes the doctor completely relies on the result of an X-ray or MRI scan and does not consider it necessary to check it again himself.At the same time, manual examination can reveal overlooked details and identify comorbidities that also require treatment.
If gonarthrosis is suspected, all examinations and observation by a doctor should preferably be carried out in a specialist orthopedic clinic.
How to treat arthrosis of the knee joint?
All treatment methods are selected individually and used in combination.You cannot use a regular joint ointment as self-medication, since its effect is only temporary and does not eliminate the cause of the disease.The optimal combination is medication, physiotherapy, proper nutrition and physiotherapy.
Hormonal medications
Steroid medications have a variety of effects on the body, including anti-inflammatory and pain-relieving effects.Such drugs are used as injections into the joint at the time of exacerbation of the disease to quickly relieve pain and swelling.The disadvantages of the method include side effects and limited frequency of use (preferably no more than once every 2 weeks).In addition, hormonal injections do not eliminate the causes of the disease, but in combination with other methods relieve the symptoms and cannot be considered a complete treatment.
Chondroprotectors
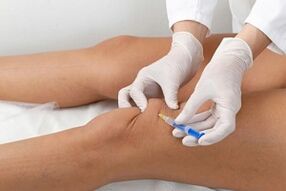
This is a group of drugs that act on the cartilage tissue, restoring and nourishing it and improving the quality of the lubricating fluid.
The most effective in the treatment of arthrosis of the knee joint are preparations containing glucosamine and chondroitin sulfate.These substances are contained in several medicines.
The attitude of doctors and patients to chondroprotectors is ambiguous.Some patients expect unrealistic quick results from the treatment thanks to advertising.If they do not find them, they become disappointed and begin to consider this group of drugs useless.
In fact, chondroprotectors require long-term use in combination with other treatment methods.
These drugs are significantly more effective in stages 1-2 of the disease and not when the cartilage tissue is already severely damaged.
Hyaluronic acid
Sodium hyaluronate is a natural moisturizing ingredient produced in the human body.Through intra-articular injections, hyaluronic acid deeply nourishes dry, thinned cartilage, restoring joint mobility and acting as an effective natural lubricant.The disadvantages of the method include the undesirability of use during periods of exacerbation, inflammation and the high price.At the same time, a well-coordinated treatment with hyaluronic acid can replace surgical intervention, which can be even more expensive.
Anoint
Gels and ointments with analgesic and anti-inflammatory effects cannot affect the cause of the disease, but can significantly alleviate the patient's condition.Warming preparations improve blood circulation, improve nutrition of the diseased area and support general treatment.Nonsteroidal anti-inflammatory ointments are often used to relieve pain, although the amount of active ingredient is relatively small and can penetrate the joint through the skin.
Diet therapy
Scientists have been studying the connection between the consumption of certain foods and joint osteoarthritis for many years.It has been suggested that the increased risk of morbidity is influenced by consumption of meat, processed foods and excessive salt, but these suggestions have not been confirmed.The only thing that has to do with food and arthritis is being overweight.Therefore, the principles of diet therapy for this diagnosis are based on the general rules of healthy eating and reducing and controlling body weight.
Recommendations for patients with knee osteoarthritis:
- Limit the consumption of ready-made meals and fast food and give preference to homemade dishes made from simple products.
- Stick to the healthy salt intake norm - no more than 1 teaspoon per day.
- Limit sweets, fatty foods, carbonated drinks and flour products.
- The diet should be varied, with the majority consisting of fruits, vegetables, grains, dairy products, nuts, eggs (especially protein) and lean meat.
- On the recommendation of your doctor, you can take a complex of vitamins and dietary supplements.
If a patient with knee osteoarthritis is already overweight, he or she needs to see a nutritionist.The specialist can give advice based on the patient's age, lifestyle and other indicators.
Folk remedies for the treatment of arthrosis
In folk medicine, infusions, decoctions, compresses from medicinal herbs and other components are used to treat joints.With the approval of the doctor, these drugs can complement the main treatment or be used to prevent gonarthrosis at the first signs of discomfort and arthrosis of the knee joint.
Several folk recipes:
- Rub with turpentine.Mix the egg yolks, a teaspoon of turpentine and a tablespoon of apple cider vinegar.Rub the mixture into the affected area overnight and wrap it in a woolen cloth.Use 1-2 times a week.
- Honey and Mumiyo.For 100g of honey you need to add 3-4g of mumiyo.Rub into knees before bed.
- Dandelion infusion.To prepare half a liter of alcohol or vodka, pour it into a dark glass container.Fill it with yellow heads and leave it in a cool place for at least a month.Rub the strained product into the sore spot before bed.
Such recipes help in complex treatment, relieve pain and inflammation, but do not replace them.Illiterate self-medication can worsen your condition.
massage
Manual and hardware massage and manual therapy are ideal for overweight, sedentary people with osteoarthritis.If there is excessive fluid accumulation in the joint, lymphatic drainage is indicated.All types of massage go well with physiotherapy and are used to relax muscles after training.Contraindications to massage are acute inflammation.
Physiotherapy
Numerous interventions using heat, cold, electric current, ultrasound and laser beams slow the progression of osteoarthritis, improve blood circulation in the affected area and have an anti-inflammatory and pain-relieving effect.
Most often the doctor prescribes:
- Shock wave therapy.The method involves directing sound waves specifically to the area of the diseased joint.This effect relieves swelling, improves cartilage nutrition and destroys salt deposits.The most effective method of physiotherapy for osteoarthritis.
- Myostimulation.Electrical impulses relieve cramps and muscle tension and maintain mobility of the knee joint.
- Phonophoresis.This therapy combines the local action of ointments and gels with ultrasound.This increases the penetration of useful substances into the skin.
Cryotherapy, paraffin therapy, laser therapy, magnetic field therapy and other techniques are less commonly used.
Kinesitherapy
Popular techniques include physical therapy and joint traction.The exercise therapy complex is prescribed individually by a rehabilitation doctor.This can include exercises with weights, medical equipment and gymnastics to improve independent performance.Some exercises need to be done in bed in the morning, others 3-4 times a day.The effectiveness of therapeutic exercises largely depends on the patient's responsibility and his desire for recovery.If done correctly, such physical training will help stop deterioration and prevent surgery.
A special orthopedic device is used for traction.This method allows you to increase the gap between the joints, reduce their friction and the load on the sore knee.
Surgical treatment
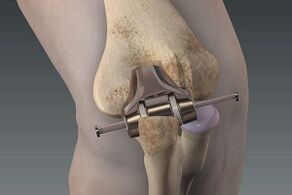
Osteoarthritis surgery is a method of addressing the cause of the disease and not just the symptoms.It is used in stages 2-3 of arthrosis when other methods are ineffective.There are several intervention options:
- Arthroscopy.Modern methods allow the operation to be performed through small incisions using thin instruments under the supervision of a video camera.This type of surgery is easier to tolerate and recovery is faster.During the operation, the surgeon removes destroyed cartilage and tissue fibers.
- puncture.Refers to low-traumatic interventions.Excess fluid is pumped out of the joint using a syringe.Allows you to relieve swelling and inflammation and increase mobility.
- Endoprosthetics.If the joint is already severely damaged in the final stage of osteoarthritis, it can be replaced with a titanium joint that is compatible with the body.This is the most extensive procedure, followed by long-term rehabilitation.They resort to it in the most difficult cases, when there is no other option.
To avoid surgery, you need to monitor your health and start treating diseases at the initial stages.There is no need to endure pain in the knee joint and other signs of osteoarthritis for years and drown it out with painkillers.
Preventive measures for osteoarthritis of the knee joint
You need to start taking care of the health of your knee joints early.The older you are, the more preventive measures you need to take.Athletes and overweight people should pay particular attention to the musculoskeletal system.
To prevent arthrosis of the knee joint, you must:
- Choose sports and loads correctly according to your abilities.
- Use comfortable, high-quality, low-heeled shoes.
- Swimming that stresses and relaxes all muscles and joints evenly.
- Avoid joint injuries and complete their treatment.
- Avoid excessive weight gain and keep it normal.
In addition to lifestyle adjustment, timely treatment of congenital features of joint development, for example, various deformities and dislocations, is important.
Osteoarthritis of the knee joint can occur not only in older but also in young patients.The disease takes a long time to develop and with the right approach it is possible to recover and avoid serious health consequences.
















































